More pages in this section
Heel Pain (Plantar Fasciitis)
Plantar Fasciitis is the most common cause of heel pain and also the most common condition presenting to our Townsville Podiatry clinic. That being said, heel pain can be quite a complex condition that needs to be correctly diagnosed and treated specific to each person.

What is Plantar Fasciitis?
The plantar fascia is a thick fibrous band of tissue in the bottom of the foot which runs from the heel to the base of the toes. When placed under sudden or continual increased strain/load, the plantar fascia can become injured generally at the point where it inserts into the heel bone. This is usually a slow onset of pain with no ‘one-time’ injury required.
By adulthood many people will have developed a heel spur in both heels. It’s important to note that in many of cases of heel pain, the heel spur is not the cause of the pain. The pain is due to an injury to the soft tissue (plantar fascia), regardless of whether a heel spur is present or not.
Do you suffer from Plantar Fasciitis heel pain? Contact us today to make an appointment.
Signs & Symptoms of Plantar Fasciitis Heel Pain
- Pain under the heel which may extend into the arch
- Heel pain is usually worse the first few steps in the morning and after rest periods during the day
- Heel pain often aggravated by prolonged standing, walking or running, especially on hard surfaces
- As the condition progresses, patients may experience burning, numbness and throbbing around the heel when resting at night
Causes of Plantar Fasciitis or Heel Pain
Often there has been an increase in load placed on your lower limb that your body has not had the capacity to deal with resulting in injury. This increase in load may include:
- Jobs that require lots of walking on hard surfaces
- Prolonged barefoot on hard surfaces (often happens when people are on holidays for a few weeks)
- Starting a new exercise program; or increasing your training intensity/volume or style
- Weight gain
- Wearing old, worn out footwear; high heels
Certain foot types may increase your likelihood of developing heel pain – or put more simply – feet that do not work too well. Whether that be collapsed arches, tight calf muscles, weak intrinsic foot muscles, high arch rigid feet with poor shock absorption etc.
Certain factors may increase the risk of developing heel pain and/or impair your body’s own ability to repair the injury – such as Diabetes, Rheumatoid Arthritis, menopause, obesity, old age, stress, inadequate sleep.
There may be more involved than just the Plantar Fascia
As mentioned earlier, heel pain can be quite complex. A more recent and appropriate term is Plantar Heel Pain - pertaining to pain on the bottom of the heel. So this will often involve injury to the plantar fascia in either an inflammatory process (plantar fasciitis) or a degenerative process (plantar fasciosis). The plantar fat pad may become bruised, the plantar calcaneal bursae may be inflamed and irritated. A plantar spur may be contributing to symptoms. The calcaneus (heel bone) may have bone oedema. A branch of the medial calcaneal nerve may be compressed causing heel pain (Baxter's neuropathy). The plantar fascia may not even be involved. Often the longer the heel has been sore, more of the above issues come into play.
Our experienced Podiatrists are able to refer for medical imaging to assist with our diagnosis. Together with thorough questioning and a detailed assessment we are able to make an informed decision as to the most appropriate treatment plan.
Heel Pain Treatment Options
Like most over-use soft tissue injuries – our approach at Foundation Podiatry to managing Heel Pain is to "calm it down – build it up".
So what do we mean? The initial focus is to reduce the load / strain on the injured plantar fascia to allow the body to start its own healing process. This may involve strapping, suitable footwear, Custom Foot Orthoses, night socks/splints or even a moon boot (depending on the severity of your heel pain). Physical activity may need to be reduced or modified – cycling instead of running for example.
Once the heel pain starts to improve we then focus on improving the function of the foot and lower limb. Mobility, balance and strength exercises need to be introduced at the right time.
Depending on your individual case however we may need to include another step which is an assistance with tissue healing. Ask yourself - How long have you had heel pain? How much time do you spend on your feet each day? How capable is your body of healing itself (stress levels, appropriate sleep and nutrition). What is your body weight etc.
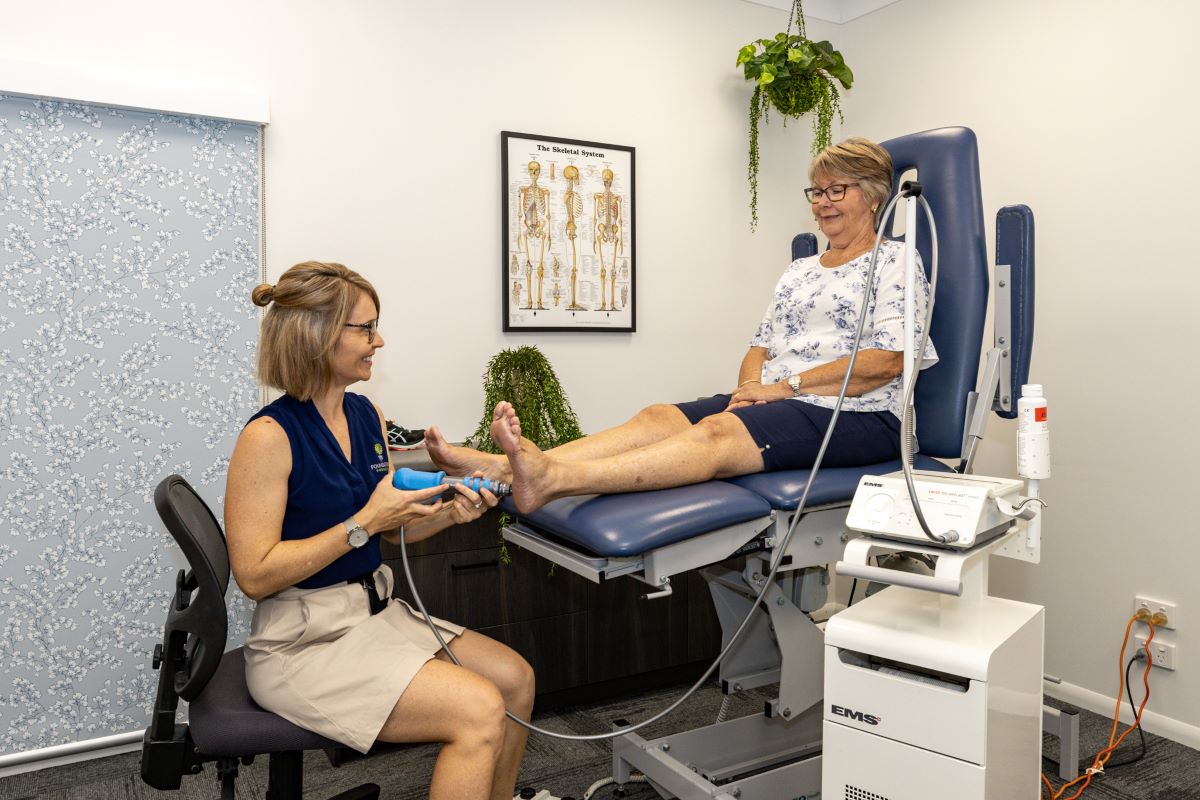
Depending on the above and whether your heel pain is presenting in an acute or chronic stage – an assistance in tissue healing such as Shockwave Therapy, Prolotherapy Regenerative Injection Therapy or Medical Acupuncture may be required to settle your heel pain completely.
Plantar Heel Pain is a common condition yet complex in nature, where a 'one size fits all treatment approach' often fails. An accurate diagnosis is important to prescribe the most suitable treatment plan.
[feature-block]
Tired and grumpy due to heel pain?
Ready to live an active lifestyle again?
Want to learn more about Plantar Fasciitis heel pain treatment?
Make an appointment with our experienced Podiatrist Hayley today!
Book Now
[/feature-block]










